June 8, 2018, by NCI Staff

Travis Carpenter, who received the drug selumetinib to treat NF1, with Zilly, a therapy dog at The Children’s Inn at NIH.
Credit: National Cancer Institute
An investigational drug called selumetinib can shrink tumors in children and young adults with a genetic syndrome called neurofibromatosis type 1 (NF1) and may improve symptoms such as pain and reduced mobility that result from tumors called plexiform neurofibromas, which develop in many people with NF1, according to preliminary results from a clinical trial.
The phase 2 trial, which involves 50 patients aged 2 to 18 with NF1 and plexiform neurofibromas, confirms the results of a smaller trial that in 2016 demonstrated for the first time that the drug could shrink large tumors.
Up to half of all patients with NF1 develop plexiform neurofibromas, which form in nerve cells. Although most of these tumors are not cancerous, they typically grow on or just under the skin, causing pain and other problems such as difficulty breathing or walking and disfigurement.
“The new results are exciting because they confirm what we learned in the phase 1 study, where, for the first time in this disease, we saw large tumors shrink,” said Andrea M. Gross, M.D., of NCI’s Center for Cancer Research, who presented the findings June 2 at the American Society of Clinical Oncology annual meeting in Chicago.
In a message on Twitter, NCI Director Ned Sharpless, M.D., also called the results “exciting.” He summarized the findings on Twitter: “Tumors shrink, kids feel better, drug seems safe.”
Confirming that Selumetinib Can Shrink Neurofibromas
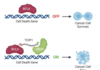
Selumetinib, which is taken as a pill, blocks a protein called MEK that is part of the RAS signaling pathway in cells. This pathway is improperly activated in patients with NF1 as well as in patients with certain types of cancer, leading to the growth of tumors.
In the trial, 36 of the 50 patients (72%) had a partial response to selumetinib, meaning that tumor volume shrank by at least 20%. This result was essentially the same as in the smaller phase 1 study published 2 years ago, in which 17 of 24 patients (71%) had a partial response.
In the current trial, the median change in plexiform neurofibromas volume from baseline was -27% (the range was from -50.6% to 2.2%), the researchers reported. The median age of patients in the trial was approximately 10 years old.
Plexiform neurofibromas grow most quickly in young children with NF1 and then slow down during adolescence, according to Brigitte Widemann, M.D., chief of NCI’s Pediatric Oncology Branch and a leader of the study, whose team also developed a method of measuring the volume of tumors.
Before treatment, the most common NF1-related health problems in the patients were disfigurement (44 patients), motor dysfunction (33 patients), and pain (28 patients).
Some plexiform neurofibromas grow to be as large as a several-liter bottle and up to 20% of body weight. Surgery to remove even small tumors is often not feasible, because many tumors are intertwined with healthy nerves and tissue. In addition, tumors that have been partially removed by surgery tend to grow back, especially in young children.
The side effects of selumetinib are generally manageable, noted Dr. Gross. Nausea, vomiting, diarrhea, and rashes were among the most frequent side effects in the trial, but these side effects were still relatively uncommon and improved when drug was paused. For 12 patients, the dose of selumetinib had to be reduced because of side effects, and four of these individuals eventually stopped treatment.
Assessing Health Problems Related to Neurofibromas
In addition to causing some tumors to shrink, selumetinib appeared to help improve health problems associated with tumors. After a year of treatment, most patients in the trial (or their parents) reported improved pain scores, strength, and range of motion, Dr. Gross noted.
“In this trial, we’re trying to show if selumetinib produces a clinical benefit—that is, that the patients are feeling better and are more active than they’ve ever been with the disease,” she explained.
To this end, the researchers used multiple tests to measure changes in a patient’s health and ability to function during treatment. Patients return to the NIH campus for evaluations on a regular basis, allowing the researchers to monitor a range of health measures.
“This is a unique and resource-intensive study in terms of the level of detail in the functional and patient reported assessments of patients,” said Dr. Gross. In addition to the clinical testing, patients provide anecdotal information that gives the researchers a richer view of how the treatment has changed their everyday lives.
“One patient explained that his clothes fit better after being on the medicine, and another said that he was able to wrestle his sister again,” Dr. Gross recalled. “Parents and the neurofibromatosis type 1 community are excited about this trial because patients for the first time see benefits from the treatment of large plexiform neurofibromas.”
After Dr. Gross shared the results in Chicago, the mother of a study participant wrote on Twitter that her son’s “tumor is no longer threatening the airway, and we can see down his throat again. Not to mention the psychosocial impact of kids not asking about his neck anymore.”
The mother of another participant in the trial tweeted that her son’s tumor was shrinking and that he was feeling better with less pain and more energy. The biggest side effect, she added, was “blond hair.”
Exploring Unanswered Questions
In February, the Food and Drug Administration (FDA) granted “orphan drug” status to selumetinib for the treatment of patients with NF1. This designation allows drug developers—in this case, AstraZeneca and Merck—to receive incentives such as tax credits and exclusive marketing rights for a period of years.
During the phase 2 trial, some tumors stopped responding to selumetinib and began to regrow, particularly after the dose of the drug was reduced in patients experiencing side effects. It appears that a certain dose of selumetinib is needed for shrinkage of plexiform neurofibromas. More research is needed to understand why some tumors may show growth despite an adequate dose of selumetinib.
Some clues may emerge from an NCI-sponsored clinical trial testing selumetinib in adults with NF1, Dr. Gross said. The adult participants in that study are providing serial tissue samples, which could help the researchers gain insights into mechanisms of response and possible resistance mechanisms.
Dr. Widemann, Dr. Gross, and their colleagues will continue to follow the younger patients in the phase 2 pediatric study and the adult patients as well.
“We’re incredibly grateful to the patients and their families who come and do all of our intensive evaluations,” said Dr. Gross. “We think that we’re making a clinical difference for many patients and are pleased to be documenting these changes in a prospective study.”