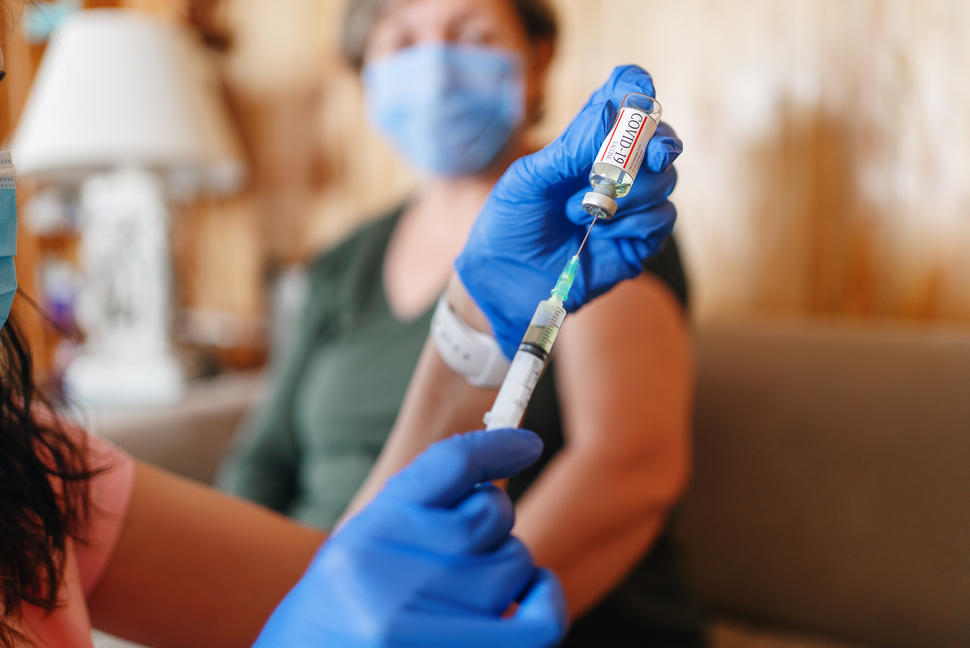
, by Edward Winstead
People with cancer who are treated with certain immunotherapy drugs can receive mRNA COVID-19 vaccines without an increased risk of immune-related side effects, new research suggests. The findings are in line with the results of earlier, smaller studies.
The new study involved more than 400 people with cancer who were treated at Memorial Sloan Kettering Cancer Center (MSKCC). Each received an mRNA COVID-19 vaccine before or after treatment with a type of immunotherapy drug known as an immune checkpoint inhibitor.
An analysis of the patients’ medical records revealed no evidence that mRNA COVID-19 vaccination had increased the type, frequency, or severity of immune-related side effects, such as inflammation in the lungs or colon, researchers found.
“It is safe for people to receive immune checkpoint inhibitors and COVID-19 vaccines,” said Adam Widman, M.D., who was part of the research team. “We hope our findings will allay concerns about immune-related side effects among patients as well as oncologists.”
There were no signs of increased immune-related side effects among specific groups of patients in the study (e.g., older patients or those with a specific cancer type), the researchers reported in the October issue of the Journal of the National Comprehensive Cancer Network.
“This is an important study,” said James Gulley, M.D., Ph.D., who codirects NCI’s Center for Immuno-Oncology but was not involved in the research.
“The findings add to what is known about the safety of giving COVID-19 vaccines to people taking immune checkpoint inhibitors, which are an important treatment option for a growing number of patients with cancer,” Dr. Gulley added.
Medical groups recommend COVID-19 vaccines for people with cancer
People with cancer have a higher risk of severe complications from COVID-19. Approved vaccines against SARS-CoV-2 have been shown to reduce the risk of hospitalization and death from COVID-19 among people with cancer.
The Centers for Disease Control and Prevention (CDC) and other medical groups generally recommend that people with cancer receive an mRNA COVID-19 vaccine.
But some people with cancer have been reluctant to be vaccinated while being treated with immune checkpoint inhibitors out of concerns that the additional stimulation of the immune system could contribute to side effects.
“Some clinicians and patients at Memorial Sloan Kettering had concerns that the COVID-19 vaccine might interfere with immunotherapy and might spur immune-related adverse events, which can be serious,” said Dr. Widman.
“Fortunately, we found no evidence to support those concerns,” he added.
Providing reassurance about the safety of COVID-19 vaccines
People with cancer were not included in the initial studies of the mRNA COVID-19 vaccines. As a result, when the vaccines became available there were no studies of these vaccines in patients receiving immune checkpoint inhibitors.
Studies of other vaccines have suggested that patients undergoing treatments for cancer that involve suppressing the immune system, such as stem cell therapy, should hold off on vaccination for several months because the response to the vaccine may be temporarily lessened.
In terms of side effects, a 2019 study found that the flu vaccine did not contribute to increased immune-related side effects in patients being treated with immune checkpoint inhibitors. The flu vaccine study was led by Mini Kamboj, M.D., the chief medical epidemiologist at MSKCC, who also led the new COVID-19 study.
Two studies published in 2021 also found no signs that COVID-19 vaccines contribute to immune-related side effects. One study was conducted in Israel, and the other in the United States. The MSKCC study was larger and followed patients for longer after vaccination than the earlier studies did.
The new findings should provide additional reassurance to doctors and patients about the safety of COVID-19 vaccines, noted Ido Wolf, M.D., of Tel Aviv University, who led the Israeli study.
“These vaccines can save lives, particularly for patients with cancer who may be older and have weakened immune systems and other health conditions,” said Dr. Wolf.
Most of the immune-related side effects were mild
The 408 patients in the MSKCC study had received a first dose of an mRNA COVID-19 vaccine within 90 days before or after receiving an immune checkpoint inhibitor.
Most patients in the study received the Pfizer-BioNTech vaccine, and their median age was 71 years old. The patients had many different types of cancer.
The immune checkpoint inhibitors they received included pembrolizumab (Keytruda), nivolumab (Opdivo), ipilimumab (Yervoy), and combinations of these drugs. During the follow-up period (90 days from vaccination), the researchers found:
- 27 patients (7%) experienced a new immune-related side effect, such as a rash, diarrhea, or colitis. Most of the side effects were mild.
- 4 patients (1%) developed severe immune-related side effects. In all cases these side effects were gastrointestinal, either colitis or diarrhea.
- None of the 28 patients who received the first vaccine dose and immune checkpoint inhibitor on the same day developed an immune-related side effect.
- 3 of the 54 (6%) patients with a history of immune-related side effects prior to getting vaccinated had an immune-related side effect after vaccination.
- 9 of the 52 (17%) patients who began an immune checkpoint inhibitor after vaccination developed an immune-related side effect.
Patients who started a new immune checkpoint inhibitor during the follow-up period were more likely to experience an immune-related side effect than other patients in the study. A limitation of the study was the lack of a comparison group of people who received immunotherapy but were not vaccinated, the researchers noted.
A clear message: “The vaccines are indeed safe”
The rate of immune-related side effects in vaccinated people treated with immune checkpoint inhibitors in the current study is similar to rates of these side effects in unvaccinated people treated with immune checkpoint inhibitors, according to the researchers.
Developing reliable evidence on the safety of COVID-19 vaccines in people with cancer is extremely important, noted Dr. Wolf. “Concerns about the safety of these vaccines are often based only on theoretical speculation and are not supported by the evidence,” he said.
But the message of the new study, he continued, “is loud and clear. The vaccines are indeed safe and should be given to patients with cancer who are treated with immunotherapy.”
The new findings have been “tremendously useful” at MSKCC in recent months, Dr. Widman noted. “Doctors have been reassured by the results, and they have recommended the vaccine to their patients receiving immunotherapy.”