The pace of progress in cancer research keeps getting faster and faster. However, the results of this research can take time to reach the medical community. The ASCO Plenary Series is a program developed by the American Society of Clinical Oncology (ASCO) to help speed the delivery of high-impact cancer research. In this series, cancer care providers gather online to learn about new, carefully selected research and discuss the study results with their colleagues.
The January 2023 session in the ASCO Plenary Series features this study:
Follow the discussion about research from the ASCO Plenary Series by using the #ASCOPlenarySeries hashtag on Twitter.
Using a blood-based test to select treatment for advanced gastrointestinal stromal tumors (GISTs)
Who does this study affect: People with advanced GIST who cannot continue taking imatinib (Gleevec).
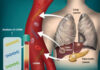
What did this study find: A GIST is a specific type of tumor that forms in the gastrointestinal tract, which is the body’s system for digesting food. GISTs are part of a group of cancers called sarcomas, which begin in tissues that support and connect the body. There were an estimated 4,000 to 6,000 people diagnosed with a GIST in the United States in 2022.
The targeted therapy drug imatinib is often the first drug used to treat people with GIST, also called first-line treatment. But for people with advanced GIST whose tumor has not been stopped by imatinib or who cannot continue taking the drug, often because of side effects, different treatment is needed. When this is the case, it is called second-line treatment. The current second-line standard of care treatment for advanced GIST is sunitinib (Sutent), which is a drug that targets the KIT gene and stops blood vessel growth in tumors. If sunitinib no longer works to treat the GIST, then other targeted therapies, including ripretinib (Qinlock), may be used.
The phase III INTRIGUE clinical trial was an international study designed to test whether ripretinib was more effective at treating advanced GISTs than sunitinib after imatinib could no longer be used. As discussed in an ASCO Plenary Series session from 2022, this study’s original analysis found that ripretinib was found to have similar effectiveness as sunitinib as a second-line treatment for GIST.
In this new, additional analysis from the same clinical trial, the researchers used a blood test to detect fragments of tumor DNA in the body, called circulating tumor DNA or ctDNA. They then analyzed the ctDNA for specific mutations in the KIT gene. This kind of test is sometimes referred to as a liquid biopsy. The researchers wanted to know if ripretinib or sunitinib worked better depending on the specific type of KIT mutation found in the tumor and examined in tumor DNA shed into the blood.
This analysis included 362 tissue samples. Of those 362 samples, ctDNA was detected in 280 of them (77%), and in those samples, 213 had KIT mutations (76%). The 2 most common KIT mutations affected the exons 13 and 14 and exons 17 and 18. An exon is a specific segment of DNA.
The researchers found that sunitinib worked better when there was an exon 13 and 14 mutation on the KIT gene. Tumor growth was stopped for 15 months by sunitinib, compared with 4 months by ripretinib. About 15% of people in the study had their tumors shrink with ripretinib, compared with 10% of people who had their tumors shrink with sunitinib.
But when there was an exon 17 and 18 mutation, ripretinib worked better. Tumor growth was stopped for around 14 months by ripretinib, compared with about 2 months by sunitinib. Tumor shrinkage occurred in 44% of people who received ripretinib, compared with none for the people who received sunitinib.
What does this mean for patients: For people with advanced GIST that is no longer effectively treated with imatinib, using a blood test to detect ctDNA may be useful for choosing which second-line targeted treatment may provide the best results.
Read this abstract and authors’ disclosures on ASCO.org.
“This non-invasive blood test may be a highly meaningful tool to select the most effective drug in patients with GIST who progressed while receiving the first-line treatment with imatinib. Our analysis shows that patients with concurrent mutations in KIT exons 11 + 17/18 in the absence of other mutations showed even better overall survival when treated with ripretinib compared to those treated with sunitinib. We plan to validate these data in a new, pivotal phase 3 study. Apart from that, the magnitude of this difference suggests plasma testing to become part of routine care for patients with GIST in the future.”
—lead study author Sebastian Bauer, MD
University Hospital Essen
Essen, Germany