March 8, 2019, by NCI Staff
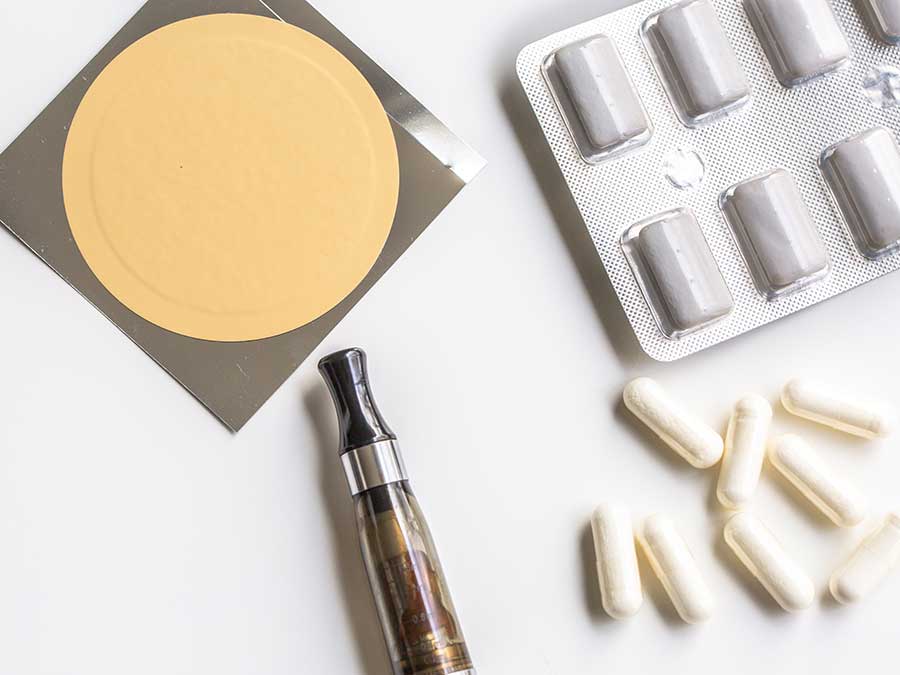
In a UK study, e-cigarettes plus counseling were more helpful to smokers trying to quit tobacco than counseling and nicotine replacement products, like patches and gum.
Credit: iStock
Cigarette smokers provided with electronic cigarettes (e-cigarettes or vaping) and smoking cessation counseling had higher quit rates than smokers given nicotine replacement therapies, such as patches, gums, and lozenges, together with face-to-face smoking cessation counseling, results from a randomized clinical trial conducted in the United Kingdom (UK) show.
At one year following enrollment in the study, 18% of the smokers who were provided with refillable e-cigarettes had stopped using cigarettes, compared with 9.9% of the smokers who were provided with nicotine-replacement therapies.
The results were published February 14 in the New England Journal of Medicine.
“Many smokers report finding e-cigarettes a helpful way to quit smoking, but there have been few randomized trials conducted to show this, and none with a more advanced, refillable e-cigarette,” said study coauthor Dunja Przulj, Ph.D., of Queen Mary University of London. Dr. Przulj added, “This is the first study to show that refillable e-cigarettes can help people to quit smoking.”
“This was a rigorous and well-conducted trial, which informs an important question: Are e-cigarettes effective for helping smokers quit cigarettes, compared to evidence-based smoking cessation medications?” said Rachel Grana, Ph.D., M.P.H., of NCI’s Tobacco Control Research Branch (TCRB), who was not involved in the study.
“Although the study contributes data to help answer this question, the findings will need to be confirmed in other settings and contexts,” she cautioned, “and there are features of the study that caution against a broad interpretation of the effectiveness for e-cigarettes for smoking cessation.”
Broader Context of the Findings
The clinical trial enrolled 886 adult smokers (median age 41) who sought help with quitting cigarette smoking through the National Health Service’s (NHS) stop-smoking service, which is available for free to smokers in the United Kingdom.
Each participant was randomly assigned to receive e-cigarettes or the nicotine-replacement therapies of his or her choice. Participants also received the standard four weeks of NHS stop-smoking service’s individual, face-to-face counseling with a local clinician trained to guide people through the process of quitting smoking.
After one year, 79 participants in the group assigned to use e-cigarettes (18%) and 44 participants in the group assigned to use nicotine-replacement therapy (9.9%) had quit cigarette smoking (as validated by a chemical breath test).
Participants in both groups rated their assigned product (e-cigarettes or nicotine-replacement therapy) as less satisfying than cigarettes. However, participants who were assigned to use e-cigarettes reported that e-cigarettes provided them with greater satisfaction and rated them as more helpful to refrain from smoking than participants in the nicotine-replacement therapy group rated their product. Overall, side effects in both groups were mild, the researchers found.
The findings needed to be considered in a broader context, Dr. Grana said. For example, participants were enrolled through the NHS stop-smoking service, so they were motivated to quit. They also received evidence-based cessation counseling in addition to e-cigarettes or nicotine replacement therapy.
In addition, the policy and regulatory environment with respect to both e-cigarettes and tobacco products in the UK is very different than it is in the United States, she continued.
“For example, the UK limits the amount of nicotine permitted in e-cigarettes and has more restrictions on e-cigarette advertising and marketing than the US,” Dr. Grana said. “So, the findings of the current study may only be applicable to smokers who want to quit and receive the recommended counseling support. They also may not be generalizable to all e-cigarette products, or to different policy and regulatory contexts.”
Long-Term Use Concerns
An important finding of the trial was that the proportion of participants in the e-cigarette group who quit smoking but continued to use e-cigarettes at one year was much greater than the proportion of participants in the nicotine replacement group who continued to use nicotine replacement therapies after one year, Dr. Grana added.
Among participants who had stopped smoking cigarettes at one year, 63 of 79 (80%) in the e-cigarette group were still using e-cigarettes; in contrast, only 4 of 44 (9%) in the nicotine-replacement product group were still using these products.
“The sustained use of e-cigarettes by the quitters in the e-cigarette treatment group highlights the need to understand the potential health effects of long-term e-cigarette use, which are currently unknown,” Dr. Grana stated.
E-cigarettes may provide some of the sensations smokers used to derive from smoking and help ex-smokers avoid withdrawal discomfort and probably prevent relapse, as well, the study authors wrote.
“E-cigarettes are also easily available, and so it is reasonable to expect that some ex-smokers will continue to use them, temporarily at least,” after they stop smoking, Dr. Przulj said.
In lab studies, including those in human cells and animals models, e-cigarette aerosol has been shown to have “potentially adverse biologic effects,” Belinda Borrelli, Ph.D., and George T. O’Connor, M.D., of Boston University, wrote in an editorial accompanying the study. “Although toxin levels and biologic effects are generally lower than those of tobacco smoke.”
As a result, they argued that the potential effectiveness of e-cigarettes in helping smokers quit must be balanced against known and potential safety concerns and that the trial’s findings “must be considered in the context of FDA-approved medications for smoking cessation that have acceptable safety profiles.”
They recommended that “e-cigarettes be used only when FDA-approved treatments (combined with behavioral counseling) fail, that patients be advised to use the lowest dose [of nicotine] needed to manage their cravings, and that there be a clear timeline and ‘off ramp’ for use.”
They also recommended that health care providers monitor their patients use of e-cigarettes, “like other pharmacologic smoking-cessation treatments.”
Potential Implications for Youth
Adult use of e-cigarettes has potential implications for younger populations, Drs. Borrelli and O’Connor wrote. Adult use exposes children to e-cigarette aerosol, and also “models addictive behavior,” they continued.
The US Surgeon General recently declared e-cigarette use among youth an epidemic, with the use of e-cigarettes among US high school students nearly doubling from 2017 to 2018 (11.7% to 20.8%).
“We’ve seen a sizeable increase in the use of e-cigarettes among youth, and there are negative health effects associated with this use,” said Dr. Grana.
For example, a recent study found that adolescents who regularly used pod-style e-cigarettes had higher levels of nicotine in their bodies than have previously been found in adolescents who regularly smoked conventional cigarettes. The Surgeon General’s report highlighted that “nicotine exposure during adolescence can cause addiction and can harm the developing adolescent brain.”
As with other tobacco products, “youth can develop nicotine addiction from using e-cigarettes and there is substantial evidence that youth e-cigarette use increases the likelihood of future use of conventional cigarettes,” explained Dr. Grana.
Constantly Evolving Landscape
“It will be important to understand how these findings translate from the controlled setting of a clinical trial to the real world where people use e-cigarettes in various ways, including without behavioral support for cessation, and for reasons other than quitting smoking,” Dr. Grana said. “We also need to better understand both the short- and long-term health effects of e-cigarette use.
“Researchers who study e-cigarettes must also contend with the broad range of products on the market,” she continued. “There are hundreds of e-cigarette devices on the market as well as a myriad of liquids with different nicotine concentrations and flavors—and the marketplace is continually changing.”
The study authors also noted that additional “trials are needed to determine whether our results generalize outside the UK [stop-smoking] services,” they wrote. For example, they called for e-cigarette cessation studies “that compare different levels of [cessation counseling] support.”