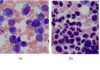
Ductal carcinoma in situ (or DCIS) is a condition where some of the cells lining the ducts of the breast tissue have started to turn into cancer cells. It’s an example of something known as a pre-invasive cancer – the abnormal cells are all contained inside the lining of the ducts, but have the potential to spread into the surrounding tissue.
In the UK, around 6,900 women are diagnosed with DCIS each year – for many, a symptomless condition that is being picked up more and more thanks to the mammograms that form part of the UK’s breast cancer screening process.
In 30 – 40% of cases, people with DCIS choose to have either part or all of their breast removed surgically – in some cases this is followed by radiotherapy. The choice to have surgery is sometimes a difficult one for a condition that has a possibility to progress to invasive breast cancer. Although this removes the affected cells, such an invasive surgery can also have a psychological impact on people who elect to have it.
So what if we could find a way to prevent people from having to undergo unnecessary treatment by predicting if a person’s DCIS will progress into invasive breast cancer?
An international team of Cancer Grand Challenges scientists – co-funded by Cancer Research UK and the Dutch Cancer Society – are tackling this question with one of the biggest studies of its kind.
Working with PRECISION
Professor Jelle Wesseling at The Netherlands Cancer Institute leads the PRECISION project, which aims to give women with DCIS more certainty and prevent unnecessary treatment.
DCIS is not cancer per se, and as long as it remains in the breast ducts it’s not dangerous. It doesn’t spread, it doesn’t hurt. But we could see first-hand how a cancer diagnosis and needless treatment impacted our patients with DCIS, their mental health and their quality of life.
– Professor Wesseling
The PRECISION team focused on collecting and analysing existing records. In the Netherlands, all of the pathology reports from labs across the country are collected and saved. The researchers used this data and linked it to other databases, including Statistics Netherlands, containing country-wide information on things such as causes of death.
By doing this, the researchers had a clear set of information: how many women in the country had been diagnosed with DCIS, how extensive was it, what sort of treatment did they have and what happened to them in the future?
From all of the data available, the team focused specifically on women whose cancer was treated by breast-conserving surgery without any further radiotherapy.
“We focused first on the group that was treated by breast conserving surgery alone,” says Wesseling. “So breast sparing surgery, no radiotherapy. The reason that we did that was that we didn’t want to have a black box effect of the radiation that is given quite frequently after breast conserving surgery.”
By joining up all of this information, the researchers were hoping to answer one question: is there anything inside DCIS lesions that can predict who will go on to develop invasive breast cancer?
Making the prediction
The researchers were able to tease out information from this data and found something surprising.
The answers didn’t only lie in the lesions themselves, but also in the surrounding tissue.
Dr Mathilde Almekinders – had the idea to explore an area of the breast that usually goes ignored: the fat cells (adipocytes) that surround the breast ducts.
“Fat tissue is a major component of the breast. And fat tissue is not just a storage organ – it has many functions also, including hormonal functions and functions in the immune system.”
The approach paid off. The team identified two key factors driving progression of DCIS to breast cancer: the size of the surrounding fat cells and the expression of a protein known as COX-2. They found that if patients had small fat cells coupled with low levels of COX-2, their risk of developing breast cancer was very low – comparable to that of the general population.
However, individuals who had high levels of COX-2 and larger fat cells were estimated to have around a 28% chance of developing an invasive breast cancer further down the line.
Piecing the puzzle together
Despite this, the team are a little way of being able to decisively predict whether or not someone’s DCIS will progress into invasive breast cancer. But they’re a whole lot closer.
“I would say we’re closer to clinical practice and defining very specific criteria that are easy to use in daily practice to distinguish women with DCIS lesions that are most likely harmless versus the ones that have a much higher risk,” says Wesseling
Wesseling says the team had always been driven by seeing how a diagnosis of DCIS can affect people.. “There had to be a way to avoid such heavy medical interventions without compromising on an excellent health outcome. I hope we’ve found it.”
Looking forward, the researchers are already collaborating with several clinical trials on DCIS features that may help predict breast cancer risk, as part of their Cancer Grand Challenges project. They want to apply their discoveries to these other trials to see if their hypothesis holds true for other DCIS cases and to see if there are any more factors in play.
– Alex