January 30, 2019, by NCI Staff
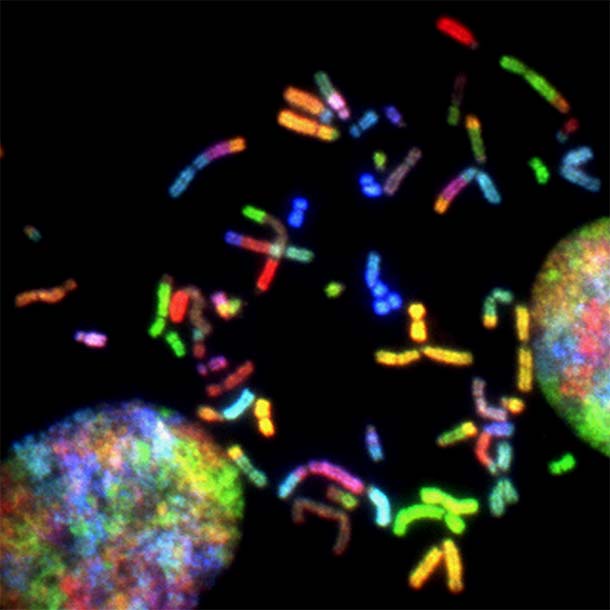
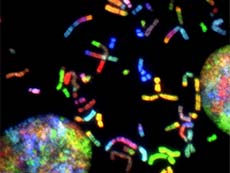
Chromosomes from glioblastoma cells. New research suggests that men and women respond differently to treatments for glioblastoma.
Credit: National Cancer Institute
Researchers have known for decades that men are more likely than women to develop an aggressive form of brain cancer called glioblastoma. There is also evidence that women tend to respond better than men to standard therapy for this disease.
The reasons for these sex differences are not clear. But a new study provides further evidence that women and men with glioblastoma appear to respond differently to treatment and identifies biological factors that might contribute to this disparity.
In the study, researchers at Washington University School of Medicine in St. Louis and their colleagues analyzed MRI results, genomic profiles of tumors, and information about survival from men and women with glioblastoma.
Using these data, the researchers uncovered different molecular profiles in the tumors of men and women and showed that these profiles were associated with differences in survival. The results appeared in Science Translational Medicine on January 2.
“Our findings and the growing body of data on the importance of sex-specific differences in biology suggest that we really need to ensure that studies are appropriately designed to detect sex differences,” said Joshua Rubin, M.D., Ph.D., of Washington University, who co-led the study.
Although researchers have been aware of substantial sex differences in the incidence of glioblastoma and other brain tumors for decades, most researchers conducting large-scale analyses have continued to merge data from patients of both sexes, Dr. Rubin added.
In future work in glioblastoma, researchers should conduct parallel but separate analyses of male and female cells, animals, and patients, noted Jingqin “Rosy” Luo, Ph.D., of Washington University, who also co-led the study.
The Biology of Sex Differences
Many diseases, including some cancers, occur at different rates in males and females or cause different symptoms depending on the patient’s sex. These differences are frequently linked to sex hormones, such as testosterone or estrogen, which contribute to many biological differences between men and women.
But males are more likely to develop malignant brain tumors than females at all ages, including in childhood. This suggests that the disparity cannot be explained solely by the effects of circulating sex hormones.
“The fact that we see sex differences in cancers in young children and young adults, as well as post-menopausal adults, means that circulating sex hormones are not responsible for the differences,” said Dr. Rubin.
When circulating sex hormones affect a disease, there are changes in the frequency and severity of the disease that parallel sex hormone levels, he continued. “That is not the case for sex differences in most cancers.”
Tracking the Growth and Spread of Brain Tumors
The current study grew out of the clinical observation that “we see a big difference in the incidence of glioblastoma between men and women and between boys and girls,” said Dr. Rubin. Males are 60% more likely to develop glioblastoma overall than females.
In the first part of the study, the researchers analyzed MRI scans and survival data for 63 adults treated for glioblastoma, including 40 men and 23 women. The patients had received surgery, followed by chemotherapy and radiation therapy.
For this analysis, the researchers, including Kristin Swanson, Ph.D., a mathematical oncologist at the Mayo Clinic, used the MRI scans and computational models to assess the growth and spread of tumors during treatment, a combined measure called tumor growth velocity.
Initial tumor growth velocities were similar for both women and men, but only women experienced a significant decline in tumor growth after treatment with the chemotherapy drug temozolomide (Temodar), which is commonly used to treat glioblastoma, the researchers found.
“The MRI studies indicated that the standard treatment for glioblastoma is more effective for females than for males,” said Konstantin Salnikow, Ph.D., of NCI’s Division of Cancer Biology (DCB), who was not involved in the study.
“Despite well-established sex differences in the incidence [of glioblastoma] and emerging indications of differences in outcomes, there are few insights that distinguish male and female glioblastomas at the molecular level or that allow specific targeting of these biological differences,” Dr. Salnikow continued.
Profiling Glioblastoma Tumors from Men and Women
To explore the molecular basis of this sex difference in treatment response, the researchers analyzed gene expression data from glioblastoma tumors included in The Cancer Genome Atlas (TCGA).
Most genes were expressed similarly in the glioblastoma tumors of men and women. But by focusing on genes that were expressed differently, the researchers found that they could separate patients with glioblastoma into five male and five female groups, or clusters. They validated the clusters by analyzing several independent data sets.
An analysis of the differentially expressed genes in the clusters showed that “survival in males was most significantly determined by genes that regulate cell division,” Dr. Rubin said. For survival in females, the most important pathway involved the expression of genes called integrins, which, he added, are involved in the spread of tumors.
Among women in the study, those whose tumors had low expression of integrin-signaling components lived, on average, slightly over 3 years after diagnosis, compared with just over a year for women whose tumors had other molecular profiles.
For men, those whose tumors had low expression of cell-cycle signaling components survived more than 18 months, on average, whereas the other tumor profiles were associated with survival of just over a year.
To explore the clinical relevance of these genetic signatures, the researchers carried out laboratory experiments in which they exposed a panel of glioblastoma cell lines from a series of male and female patients to four types of chemotherapy.
This analysis also showed associations between the cell-cycle signature and longer survival in men and between the integrin signature and longer survival in women.
Focusing on Mutations in the IDH1 Gene
The researchers also analyzed a gene called IDH1, which, when mutated, is thought to be an important driver of glioblastoma.
In previous studies, IDH1 mutations have been associated with better outcomes in glioblastoma. But in the current study, women with IDH1-mutant tumors were all in the cluster with the best survival, whereas in men, IDH1-mutant tumors were distributed in all the clusters.
“This was a very interesting result of our study,” said Dr. Rubin. “The longest-surviving female cluster was aligned with current thinking that IDH1 mutations are associated with better survival in glioblastoma. But in males that was not true.”
The finding suggests that there may be a sex-specific effect of IDH1 mutations on survival in glioblastoma, he added.
Raising Awareness about Sex Differences
“Sex differences in cancer are an understudied area of research, and more of these studies are needed to make progress in what is often known as precision, or personalized, medicine,” said Dr. Salnikow, noting that the results of the current study need to be replicated by larger studies.
Researchers can learn a lot about cancer by identifying the molecular changes driving the disease, said DCB’s Nastaran Zahir, Ph.D., who was not involved in the research.
“Looking at these molecular changes in the context of sex differences and using computational modeling approaches could enhance our ability to predict which patients are likely, for instance, to respond to treatment or to experience disease progression,” Dr. Zahir added.
Dr. Rubin cautioned that more research on sex differences in glioblastoma is needed before doctors can incorporate the approach into the clinic. He is hopeful that the current study will raise awareness about the need to pursue this area of research.
“No matter which aspect of glioblastoma we looked at, we could see sex-specific differences,” said Dr. Rubin. “As we learn more, you could imagine that treatment for glioblastoma might need to be delivered in a sex-specific manner in the future.”