Welcome to our newest blog series, “Five Questions With…” In this series, we will highlight the unsung heroes that make healthcare work. From guest services to the phlebotomist, the pet therapy volunteer, and the environmental services workers. These individuals enhance our experiences when we are getting care and highlight human connection and support. Thank you for all you do!
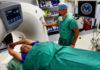
Today we feature Debra Demille, MS, RD, CSO, registered dietitian, and certified specialist in oncology nutrition. March is also National Nutrition Month! Thank you to Debra and all the other dietitians who help to educate and support patients.

How long have you been in this position?
I have been with Pennsylvania Hospital’s Abramson Cancer Center for over 22 years. In total, I have been with Pennsylvania Hospital for 34 years.
Tell us what you do to support patients.
As a Registered Dietitian who is part of the interdisciplinary team, I help patients when they are struggling with unintentional weight loss, have issues with nutrition-related symptoms (such as nausea or mouth sores) that interfere with the ability to eat as well as work with individuals when they finish cancer treatment. That is a good time to take stock and make lifestyle changes to optimize health. In addition, there are some people who can not eat by mouth thus require alternate forms of nutrition as with feeding tubes. As we know, a cancer diagnosis impacts everyone in the family or support system so I provide support and guidance for the caregivers as well.
Is there one story that sticks out in your head?
There are many stories but one has been really touching to me. A gentleman around my age was diagnosed many years ago with cancer in the throat. His treatments were difficult and he got to the point where he couldn’t eat anything at all. He was agreeable to having the feeding tube placed so I worked with his wife to come up with the best schedule to administer feedings. Over time we became close. Despite what he was going through, he always had a story and a way to make me laugh. And at a certain point, he no longer needed the tube. The cancer wasn’t done with him though and he had a recurrence and things moved to his lung. He decided since he had such a long commute to find someplace close to home but still comes back to our oncologist to review his treatment plan. Luckily with the new developments in various treatments, he is doing well. Every time he comes to our site, he asks to see me for no other reason than a hug and to catch up.
What is the most challenging part of the job?
This line of work can be stressful as many (patients) do well however, some have a limited lifespan. I am working with people in the most vulnerable time of their life so there is a lot of sharing and trust. I get to know family members, hear about grandchildren and all of the life events that make life memorable. I feel the loss when they pass.
If someone was applying for a similar position, what would you tell them about the work?
The work is so very rewarding. You can feel the impact at the end of the day. The work is varied as oncology is forever expanding in new lines of treatment. People are living longer so again, you may develop relationships over a long period of time. The work covers both the acute time of treatment and through prevention as heart disease and diabetes don’t go away when someone is diagnosed with cancer. In addition, it takes a team so I have the pleasure of working with many other disciplines such as advanced practice nurses, social workers, physicians, and more. We support the patients together and each other. Self-awareness is important as this line of work can also be emotionally draining. Finding ways to take care of yourself is important.
What is a job accomplishment that you are proud of?
I have been able to take the teaching of nutrition out of the clinical setting through cooking programs. For over 15 years, these programs were held on-site so people could use all of their senses when experiencing new foods as they could watch the recipes be prepared and then taste them. Of course with the Pandemic, the venue has changed to virtual. So we are able to reach a larger audience with people who may not be able to travel into the center of the city. Though they can’t taste the food, they can still hear all about food safety, the reasons some foods provide health-promoting properties, and ways to make cooking simpler.
Do you want to nominate a staff member, volunteer, co-worker, or friend for us to feature in “Five Questions With…” Go to oncolink.org/feedback and let us know!