A phase II/III, RELATIVITY-047, global, double-blind, randomised study evaluated dual inhibition of LAG-3 and PD-1 using a new combination of LAG-3–blocking antibody relatlimab and PD-1–blocking antibody nivolumab, as compared with nivolumab alone. Blinded independent assessment of the primary endpoint showed that progression-free survival (PFS) was longer with relatlimab–nivolumab combination than with single agent nivolumab.
The separation of the PFS curves occurred at the initial postbaseline assessment at approximately 12 weeks and was sustained thereafter. Relatlimab–nivolumab also had the PFS benefit over nivolumab in prespecified subgroups. Relatlimab-nivolumab combination showed no new safety signals. RELATIVITY-047 investigators led by Dr. Hussein A. Tawbi of the Department of Melanoma Medical Oncology, Division of Cancer Medicine, University of Texas MD Anderson Cancer Center in Houston, TX, US published their findings in the 6th January 2022 issue of The New England Journal of Medicine.
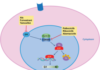
LAG-3 is a cell-surface molecule that is expressed on immune cells, including T cells, and negatively regulates T-cell proliferation and effector T-cell function. It is upregulated in many tumour types, including melanoma. LAG-3 and PD-1 are distinct inhibitory immune checkpoints that are often co-expressed on tumour-infiltrating lymphocytes. In preclinical models, dual inhibition of LAG-3 and PD-1 showed synergistic antitumour activity.
Relatlimab is a first-in-class antibody that binds to LAG-3 and restores the effector function of exhausted T cells. In a phase I/II dose-escalation and cohort-expansion study, the combination of relatlimab and nivolumab showed antitumour activity, including durable objective responses in patients with melanoma that relapsed after, or was refractory to, PD-1 inhibition.
In RELATIVITY-047, the study team evaluated relatlimab and nivolumab as a fixed-dose combination as compared with nivolumab alone when administered intravenously every 4 weeks to patients with previously untreated metastatic or unresectable melanoma.
The median PFS was 10.1 months (95% confidence interval [CI] 6.4 to 15.7) with relatlimab–nivolumab as compared with 4.6 months (95% CI 3.4 to 5.6) with nivolumab (hazard ratio for progression or death 0.75, 95% CI 0.62 to 0.92; p = 0.006 by the log-rank test). Progression-free survival at 12 months was 47.7% (95% CI 41.8 to 53.2) with relatlimab–nivolumab as compared with 36.0% (95% CI 30.5 to 41.6) with nivolumab.
Across key subgroups, PFS favoured relatlimab–nivolumab over nivolumab. Patients with characteristics that are typically associated with a worse prognosis, such as visceral metastases, high tumour burden, elevated levels of serum LDH, or mucosal or acral melanoma, had better outcomes with relatlimab–nivolumab than with nivolumab.
The authors commented that expression of LAG-3 or PD-L1 was not useful in predicting a benefit of relatlimab–nivolumab over nivolumab. In both treatment groups, the median PFS estimates were longer for patients with LAG-3 expression of 1% or greater; however, a benefit was seen with relatlimab–nivolumab over nivolumab regardless of LAG-3 expression. Among patients with PD-L1 expression of 1% or greater, median progression-free survival was similar in the two groups. A benefit of relatlimab–nivolumab over nivolumab was also observed across BRAF mutant and wild-type subgroups.
Grade 3 or 4 treatment-related adverse events occurred in 18.9% of patients in the relatlimab–nivolumab group and in 9.7% of patients in the nivolumab group. No substantial differences in health-related quality of life were noted between the treatment groups.
In an accompanied editorial, Adam E. Frampton and Shivan Sivakumar stated that as the data from the RELATIVITY-047 study mature, if the survival benefit of relatlimab–nivolumab will be similar or better than that of nivolumab–ipilimumab, it would reinforce the relatlimab–nivolumab as the new standard of care for previously untreated patients with advanced melanoma. It is unlikely that there will be a head-to-head trial between the two combinations because the difference in toxic effects.
They also commented that perhaps patients with low LAG-3 expression would derive more benefit from anti–PD-1 and anti–CTLA-4 as first-line therapy, followed by anti–LAG-3 as second-line therapy. It is needed to develop new tissue and liquid biomarkers for prediction of the efficacy and toxicity of immune checkpoint inhibitors and define the appropriate combinations and sequences of treatments for each patient.