Welcome to the fourth post in our Inequalities Series, which discusses health inequalities and how they relate to cancer, from prevention and early diagnosis to treatment and research.
In this article, we explore some of the barriers that can make it harder for some people to access cancer screening. We spoke to Dr Laura Marlow, Senior Research Fellow at King’s College London, about her research into inequalities in screening. We also spoke to Iyna Butt, who was diagnosed with stage 3 breast cancer in 2015 aged 30 and now shares her experiences to raise awareness, particularly among the South Asian community.
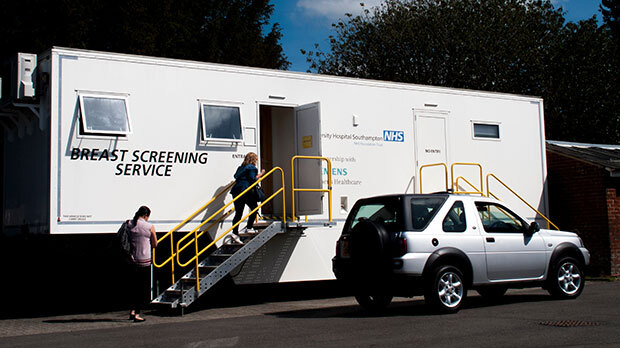
How do people access screening?
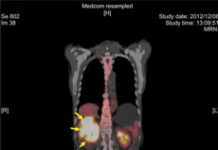
The 3 UK screening programmes, for bowel, breast and cervical cancer, save thousands of lives each year by helping to diagnose cancer at an early stage, when there are more treatment options and treatment is more likely to be successful. Cervical screening can even prevent cancers from developing in the first place.
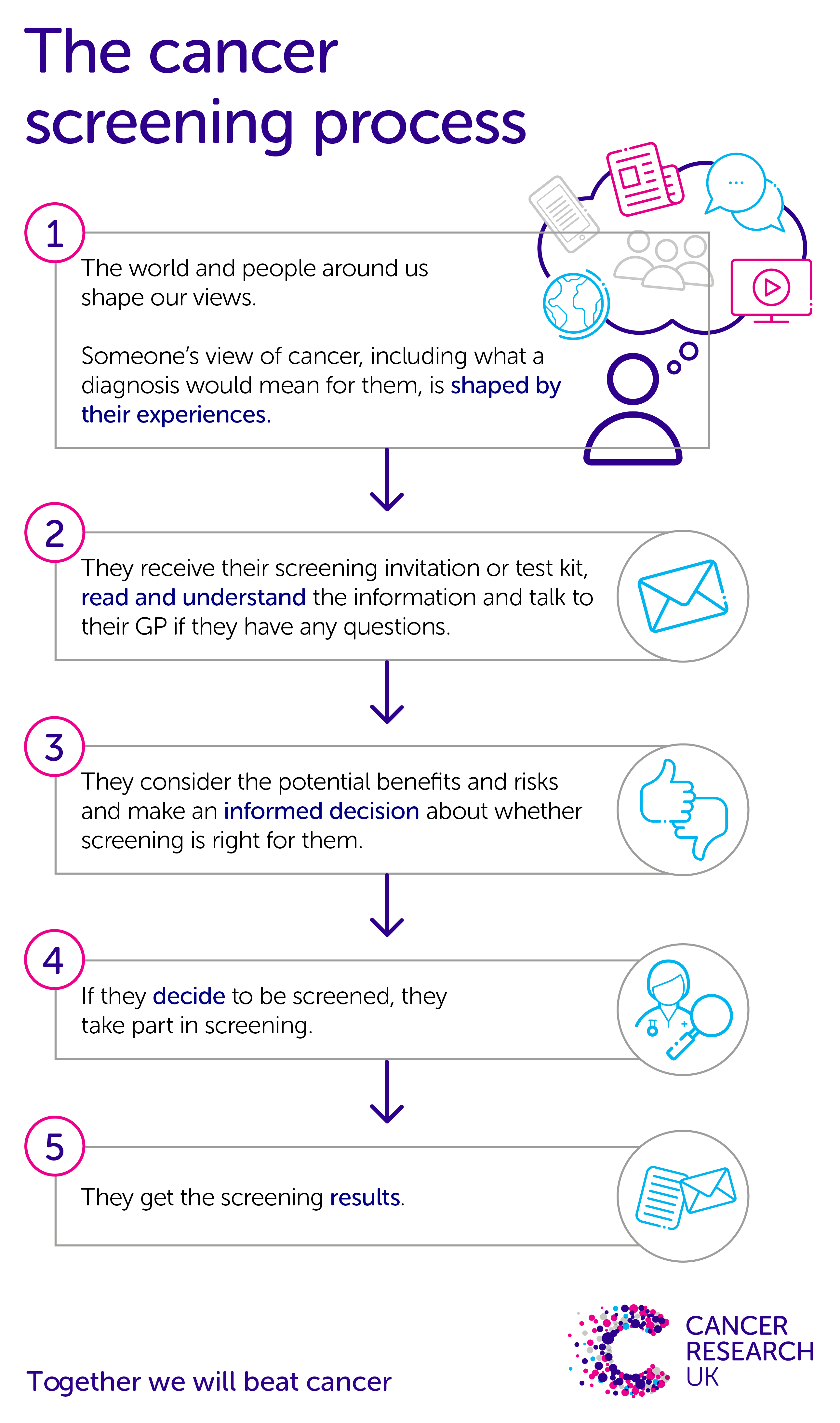
Copy this link and share our graphic. Credit: Cancer Research UK
How are barriers to screening linked to health inequalities?
In theory, almost everyone who’s eligible for screening has the same opportunities to access it. But in reality, this isn’t always the case. Informed choice is important when it comes to screening, and while someone might decide that screening isn’t right for them, there are also people who might want to be screened but something gets in the way.
When something gets in the way of screening for some groups more than others, it leads to inequalities in diagnosis, treatment and outcomes for those diagnosed with cancer. There are lots of different barriers that affect lots of different groups, and research is still uncovering the full picture. We can’t cover every barrier and group in this article, so we’re going to look at some examples of barriers that can affect someone’s attitude to screening and ability to take part if they want to.
At Cancer Research UK, our ambition is to break down barriers to screening so that everyone has equal access to prevention and early diagnosis.
Cancer stigma and screening uptake
Stigma means social disapproval of a certain characteristic and discriminatory attitudes towards people who have it.
Research has found that in England cancer stigma is linked to lower screening uptake and is more common among people from ethnic minority backgrounds. Another study found that Black people in England were less likely than White people to have their cancer diagnosed through screening. Cancer stigma may be contributing to lower screening uptake in people from ethnic minority backgrounds compared to people from White ethnic groups.
Exactly how stigma affects cancer screening behaviour is complex. However, it’s helpful to consider how fear and taboo (avoidance of something for social, cultural or religious reasons) could contribute.
“I think the stigma is a lot about fear,” explains Dr Marlow. “There’s a real overlap, fear that if you get cancer it’s a bad thing to have. People don’t talk about cancer, and if it’s not talked about, then obviously the awareness is going to be lower.”
Speaking from her perspective as part of the South Asian community, Iyna observes that conversations about cancer often only happen when someone has died from it. “It’s about knowledge and education. The only stories you’re actually hearing are because you’re at a funeral, not because you’ve heard all the positive stories of people living with cancer or people who’ve had it and survived. Because people from the community won’t talk about it.”
 100vw, 200px”></p>
<p class=) Iyna was diagnosed with breast cancer in 2015.
Iyna was diagnosed with breast cancer in 2015.
When we’re afraid of something, we sometimes develop ‘fatalistic beliefs’ about it. In general, they involve believing that there’s nothing that can be done to change an outcome. If someone believes that cancer is predetermined or ‘fate’ or always incurable, they may not see early diagnosis as beneficial. Research has found links between cancer fatalism and lower uptake of bowel cancer screening, negative attitudes to potential lung screening, low motivation to take up screening in general and later stage of diagnosis in people with lung and colorectal cancer.
Although Iyna was too young to be invited for breast screening when she was diagnosed, she confirms that this aligns with her experience in the South Asian community. “I’ve had people say to me so many times, ‘Why would I want to know? You’re going to end up dying, so what’s the point?’”
Breast, cervical and bowel cancer screening all involve intimate body parts and, in the case of bowel screening, taking a poo sample and posting it for testing. Because of this, many people find screening embarrassing, uncomfortable or unpleasant. And if there are taboos as well, these could contribute towards stigma. For example, Iyna told us that, from her experience, “It’s not seen as OK to speak about your breast or genitals or your bum. You would say, ‘I’ve got a pain in my leg or my foot,’ but you wouldn’t say, ‘I’ve got a pain in my breast.’”
One example of a taboo is where there’s a tradition of female modesty. Cervical and breast screening may be seen to breach norms and values around modesty.
Iyna explains that, in her experience, “When you see a campaign on social media or on the TV, and you see nudity, [some South Asian people] are going to scroll by, they’re going to change the channel. Nudity is not something they want to promote in their household. And when you add in cancer, you’re adding in the stigma attached to any sort of health issues, on top of it being linked to your body parts, which [have] been sexualised.”
Because cervical cancer risk is linked to a person’s sexual history, being seen to attend cervical screening and the possibility of a positive result could lead to perceptions of promiscuity and have potential social implications.
Behavioural stigma as a barrier
As well as cancer itself, if behaviours that affect cancer risk become stigmatised, this could also lead to inequalities. For example, smoking is more common among groups such as those from more deprived backgrounds, people with mental health conditions and LGBTQ+ groups.
There is a stigma attached to smoking – some people who smoke may feel judged for it. In one study in England, around 1 person in 5 agreed that screening people who smoke for lung cancer would be a waste of NHS money.
But stigmatising people’s behaviours could jeopardise the success of future screening programmes. It could mean that people from some groups are not only at higher risk of cancer, but also less likely to take up screening and be diagnosed earlier because of shame or fear of being blamed.
Practical barriers to screening
Barriers that can get in the way of attending screening, even once someone’s decided they want to go, are often practical ones. For example, it may be difficult to get to an appointment or to juggle it with other responsibilities, such as work or caring.
While these difficulties will affect most people up to a point, not everyone is equally able to spare the time and money (such as travel and childcare costs and missed wages) associated with going to a screening appointment. This can vary between groups, for example by age, socioeconomic status, gender and ethnicity.
Marlow points out that, “people often say, ‘Oh, it’s only five minutes, cervical screening,’ but it’s not only five minutes because you have to get to your GP, wait 20-30 minutes for your appointment, then you have your appointment, then you have to get the bus back. And if you need to work and are only paid for the hours that you’re working, then that’s not a luxury that you’re able to take during those hours.” So, working in a job where paid time off is available may make it easier to attend screening appointments.
Women are more likely than men to have caring responsibilities, and this can also vary by age and ethnicity. In her experience within the South Asian community, Iyna says, “We’re so family-focused, women don’t worry about their health. It’s all about caring for other people. So, when that mammogram letter comes through, even if we don’t have the stigma of body parts, we think, ‘It’s going to take me half an hour to get there, probably half an hour there, half an hour to get back, I’ve got washing to do, I’ve got to worry about who’s going to pick up the kids, forget it, it’s not important, I’m fine. And you leave it.’”
Breaking down the barriers
How the various potential barriers affect someone as they go through the screening process will be different for each individual. So, research is exploring various possible ways to tackle the issue. Combining more than one method may also be helpful, but more research is needed on this.
Research suggests that not speaking English well can be a barrier to taking up screening, so translating information could help. Actions such as making appointments more flexible and using personalised reminders and re-invitations for people who haven’t responded have been found to help increase screening uptake in underserved populations
Working with existing communities and networks could help combat fear and stigma. Marlow explains, “I think the best way for us to try and make people aware of their eligibility for screening is using existing community groups. That way, there are people who already have a rapport and can pass on those messages about how to look after health. Every interview I’ve ever done with somebody from an ethnic minority background, they’ve always been very motivated to look after their health and engage in anything that’s going to keep them healthy, but awareness of how to do this can be lacking.”
Iyna has a similar view. “What you need to do is really get to the root cause and go into the community. I use the example of childbirth. Childbirth is a conversation which is normalised. It’s seen as a part of our lives, of what we do as a woman. Within the South Asian community especially, I think it’s about normalising these conversations, and the only way you can normalise these conversations is if you go into the community.”
The way forward
It’s important to work with individuals and communities to understand the barriers that affect them and find the approaches that are effective. It’s important that any approaches are aimed at supporting people to make an informed choice and not doing anything that might make them feel pressured to take up screening if they don’t want to.
Marlow concludes, “I don’t think it’s a one-size-fits-all approach either. It might be a case of reaching out to different community groups and working with those communities to develop something that will work for that community on a local level.” For example, Marlow is involved in a study to improve screening participation amongst Muslim women.
However, it’s also not the job of local communities and groups themselves to inform people about screening and remove barriers. It’s up to the Government, the NHS, local authorities and other services to ensure that the information reaches those who need it and ensure that good practice and ideas are shared to help reduce inequalities across the different areas and services.
Research is already helping us to understand how barriers can affect access to screening for people in different groups and build strategies to reduce inequalities. Researchers like Dr Marlow are bringing us closer to breaking down the barriers.
Julia Cotterill is a health information officer at Cancer Research UK